- Foundation
- Actions
- Osteoarthritis
- Osteoporosis
- Actuality
- OAFI Radio/TV
- Get Involved
- Contact
-
-
-
OAFI
Osteoarthritis International FoundationC/ Tuset, 19 · 3º 2ª
08006 Barcelona
(+34) 931 594 015
info@oafifoundation.comSchedule:
Monday-Thursday 9AM-6PM
Friday 8AM-3PM
-
-
-

-

-

OSTEOARTHRITIS AND CO-MORBIDITIES

Article by courtesy of Dr. José Luis Llisterri Caro, Médico de Familia, Clínica Vallada de Valencia.
Osteoarthritis is a chronic disease that represents the second reason for consultation in Primary Care health centers as it accounts for 50% of visits to the doctor related to the musculoskeletal system. It is the most common joint disease and the most important cause of disability among the elderly in our country. Osteoarthritis affects all the components of the joint and causes molecular, biochemical, cellular, biomechanical and morphological changes that progressively lead to structural changes, among which are the degradation of the articular cartilage with progressive loss, the formation of osteophytes, alterations in the subchondral bone and inflammation of the synovial membrane, which are the cause of chronic pain, the “first symptom” of the disease.
The incidence of this pathology increases with age and is estimated to affect 10-20% of the population over 65 years of age. In fact, in Spain, 28% of the population over 60 years of age suffers from symptomatic osteoarthritis of the knee.
As we have been able to confirm in two studies carried out by Primary Care physicians in Spain, presented at the OAFI Cycle of Forums (Barcelona 2022) (in Spanish), it is a disease that affects mostly women (71.4%) with an average age of 68 years, with a significant overweight (75%), with obesity (50%), with osteoarthritis in various locations and with almost twice the probability of suffering from other diseases compared to patients without osteoarthritis of the same characteristics.
In the EMARTRO study we observed that osteoarthritis coexists with arterial hypertension (62.1%), high cholesterol (58.3%), type 2 diabetes mellitus (22.1%), gastroesophageal reflux (19.0%) and osteoporosis (12.2%). These patients suffer moderate pain intensity, present more problems for mobility, self-care, daily activities and present more anxiety and/or depression, resulting in a worse quality of life and, in general, a worse psychological state. The multidimensional impact of osteoarthritis highlights the need for management of osteoarthritis as a whole, including both social and psychological approaches, and not only the medical aspect of this disease.
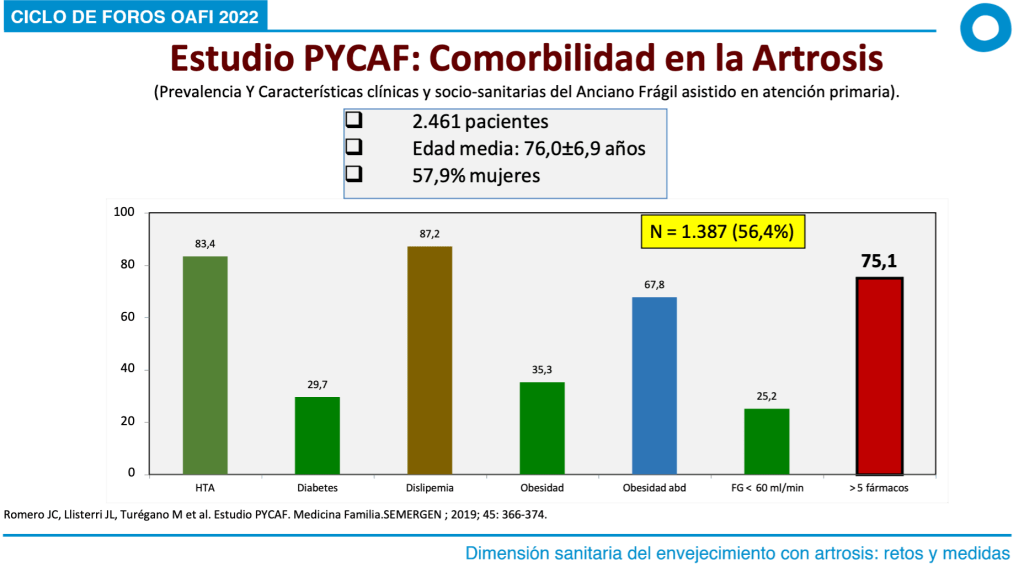
In the PYCAF study (Figure), also carried out in our country by PC physicians, osteoarthritis of any location, in patients with an average age of 76 years, was associated with dyslipidemia (87.2%), arterial hypertension (83.4%) and abdominal obesity (67.8%). Importantly, 25% of the patients with osteoarthritis had chronic kidney disease with glomerular filtration rates below 60 ml/min. This aspect is very relevant given the importance for patients with osteoarthritis of checking renal function periodically in order to avoid using drugs, such as non-steroidal anti-inflammatory drugs, which can worsen renal function in cases in which this is impaired. In the PYCAF study, we were also struck by the fact that 75% of the patients included were polymedicated, i.e., they were taking five or more drugs for their concomitant pathologies. This issue is related to what was previously commented; it is very important to pay regular attention to the renal function of all multipathological and polymedicated patients.
Another point to note is that most patients with osteoarthritis have a high cardiovascular risk. This is important when establishing pharmacological treatment because when treating our patients, one of the objectives, in addition to the effectiveness of the treatment, is patient safety. Therefore, we must avoid harmful interactions and the appearance of adverse effects.
In conclusion, osteoarthritis is a chronic and progressive disease that induces the onset of functional disability, mood disorders and loss of independence due in part to the concomitant presence of other pathologies. As a consequence, it generates important repercussions in the family, social and health fields.
Bibliographic references
- Herrero Barbero M, Giménez Basallote S, Vergara Martín J, Vilés Lladó E, Martínez Serrano H, Rodríguez Roca GC, Vergés Milano J, Llisterri Caro JL, Frías Rodríguez JF y Díaz Muñoz JA. 160/2070 – Comorbilidad asociada a pacientes diagnosticados de artrosis de rodilla en España: resultados del estudio EMARTRO. Semergen. 2015;41 (Espec Congr): 23.
- Romero Vigara, JC, Llisterri Caro, JL, Turégano Yedro, M., Cinza Sanjurjo, S., Muñoz González, L., Silvero, et al. Características clínicas y sociosanitarias en mayores de 65 años asistidos en atención primaria. Estudio PYCAF. Medicina de Familia-SEMERGEN; 2019: 45: 366-374.
Image from the article by Towfiqu Barbhuyda
Categories :